
- Call Us: 9979962669
- Email Us: drrutul.onco@gmail.com
About Us
11+
Years of Experience
25K+
Cancer Surgeries Successfully Performed
50K+
Happy Patients
Our Specialization
Our Healthcare Services
Comprehensive Cancer Medical and Surgical Solutions
Dr. Rutul Patel
About Doctor
 (3).png)
- MBBS, MS, M.Ch ( Surgical Oncology), Gold Medalist
- 11.0 Years Of Experience
- Licence No. G-24306
- In person
Testimonials
What our Patients says about us
Videos
Our Latest Videos
Media Pictures

Frequently Asked Questions
Find Answers to All Your Questions
Dr. Rutul Patel is an accomplished cancer surgeon holding an M.S. in General Surgery and an M.Ch. in Surgical Oncology. He completed his M.S. at V.S. Hospital, securing 2nd rank in the university, which equipped him with comprehensive surgical skills. Dr. Patel pursued his M.Ch. in Surgical Oncology at the prestigious Gujarat Cancer and Research Institute, where he graduated with a gold medal and first rank. His advanced training included extensive rotations in various subspecialties, such as head and neck, breast, gastrointestinal, and pediatric oncology. Dr. Patel’s qualifications are further enhanced by specialized training in minimally invasive cancer surgeries at renowned institutions like Tata Memorial Hospital and Calicut Medical College, underscoring his dedication to adopting cutting-edge surgical techniques for superior patient care.
Dr. Rutul Patel brings over a decade of experience in surgical oncology, having worked in high-volume tertiary care cancer hospitals. His expertise spans various cancer surgeries, including head and neck cancer, breast cancer, thoracic surgery, gastrointestinal cancer, gynecological cancer, and pediatric oncology. He is skilled in advanced surgical techniques, including robotic surgery and minimally invasive approaches. Dr. Patel is dedicated to providing personalized care, focusing on the latest evidence-based practices to optimize patient outcomes. His experience with diverse cancer cases has equipped him with the knowledge to handle complex surgeries effectively, ensuring that each patient receives comprehensive and compassionate care throughout their treatment journey.
Oral cancer surgery involves the removal of cancerous tissues from the mouth, including the lips, tongue, gums, and throat. The extent of the surgery depends on the cancer's size and location, ranging from excision of small lesions to partial or total removal of oral structures. Surgical procedures may also include lymph node dissection to assess potential spread. Reconstruction may follow to restore function and aesthetics, often utilizing grafts or implants. Multidisciplinary care, including consultation with oncologists and radiologists, is essential for a comprehensive treatment approach, which may also include chemotherapy and radiation therapy as needed.
After oral cancer surgery, patients may experience swelling, discomfort, and difficulty in speaking or eating. Recovery times can vary based on the extent of surgery. A diet of soft foods may be recommended initially, with gradual reintroduction of normal foods as healing progresses. Pain management and follow-up appointments are critical to monitor recovery and assess the need for additional treatments, such as radiation or chemotherapy. Speech and swallowing therapy may also be beneficial, depending on the surgical outcome. Regular follow-up visits help ensure early detection of any potential recurrence or complications.
Breast cancer surgery typically includes two main types: lumpectomy and mastectomy. A lumpectomy involves removing the tumor and a small margin of surrounding tissue, aiming to preserve the breast's appearance. In contrast, a mastectomy involves removing one or both breasts, either partially or entirely, depending on cancer's extent. Sentinel lymph node biopsy may accompany these surgeries to check for cancer spread. The choice of procedure is based on the cancer type, stage, and patient preferences, balancing effective treatment with cosmetic outcomes. Patients are encouraged to discuss options thoroughly with their healthcare team.
Recovery from breast cancer surgery varies depending on the procedure performed. Patients may experience pain, swelling, and changes in sensation in the breast area. Pain management is crucial, and doctors may prescribe medications to alleviate discomfort. Physical activity should be gradually resumed, with special attention to arm movement and stretching to prevent stiffness. Follow-up appointments are essential to monitor healing and discuss any necessary adjuvant therapies, such as chemotherapy or radiation. Support services, including counseling and rehabilitation, can aid emotional and physical recovery, helping patients adjust to changes following surgery.
Breast reconstruction surgery is performed to rebuild the breast's shape following a mastectomy or lumpectomy due to breast cancer. It can be done immediately after the cancer removal surgery or delayed until after treatments like chemotherapy or radiation are completed. The reconstruction process can involve the use of implants or autologous tissue (tissue taken from other parts of the patient's body). This surgery aims to restore the natural appearance of the breast, significantly boosting a patient’s self-esteem and overall quality of life. The choice of timing and type of reconstruction depends on the patient’s medical condition, treatment plan, and personal preference. Consultation with an experienced surgeon is crucial to determine the most suitable option for each individual.
Head and neck cancer surgery involves the removal of tumors located in areas such as the throat, larynx, mouth, or sinuses. Depending on the cancer’s stage and specific location, the procedure may include partial or total removal of affected structures. Surgeons often use advanced reconstructive techniques to restore the form and function of the treated area, which helps maintain vital activities like speaking, swallowing, and breathing. Post-surgical care usually includes rehabilitation therapy focused on speech and swallowing, assisting patients in adapting to any changes resulting from surgery. The complexity of the procedure varies, and personalized treatment plans are essential to achieve the best possible outcomes for patients.
Head and neck cancer surgery can lead to various side effects, including changes in speech, difficulty with swallowing, and alterations in appearance. These side effects often depend on the extent and location of the surgery. Post-operative rehabilitation is essential to help patients adapt and recover functionality, particularly through speech and swallowing therapy. This specialized care aids in regaining the ability to communicate effectively and manage daily eating habits. Additionally, physical therapy may be required to improve mobility and strength in affected areas. Emotional and psychological support, including counseling, can also be beneficial as patients navigate changes in appearance and lifestyle post-surgery. Early intervention and continuous follow-up care are crucial for a smoother recovery and long-term adaptation.
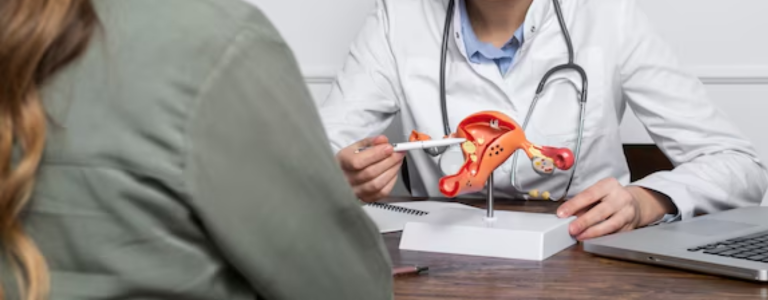
Surgeries for gynecologic cancers vary based on the type and stage of cancer. Common procedures include hysterectomy (removal of the uterus), oophorectomy (removal of the ovaries), and more extensive surgeries like radical hysterectomy, which targets surrounding tissues and lymph nodes. Depending on the diagnosis, surgeries may also involve treating cancers of the cervix, vulva, or fallopian tubes. Minimally invasive techniques, such as laparoscopic and robotic-assisted surgeries, are becoming more common due to their benefits, including shorter recovery times and reduced post-operative pain. These advanced methods provide precise treatment and often lead to better patient outcomes. Each surgical approach is tailored to the patient’s condition, balancing cancer control with preserving quality of life.
The recovery period after gynecologic cancer surgery depends on the type and extent of the procedure performed. Minimally invasive surgeries, such as laparoscopic or robotic-assisted techniques, generally result in shorter recovery times and less post-operative discomfort compared to traditional open surgeries. Patients are usually encouraged to begin gentle movement soon after surgery to reduce the risk of complications such as blood clots and to promote healing. Pain management, wound care, and nutritional support are key aspects of the recovery process. Regular follow-up visits with the healthcare provider are crucial for monitoring recovery progress and detecting any signs of recurrence. Comprehensive post-surgical care, including physical activity and lifestyle adjustments, is essential for optimal healing and long-term health.
Cytoreductive surgery with HIPEC (Hyperthermic Intraperitoneal Chemotherapy) is an advanced procedure used primarily to treat peritoneal malignancies such as ovarian or colorectal cancer. The surgery involves removing all visible tumors from the abdominal cavity, followed by the administration of heated chemotherapy directly to the area. This direct approach allows high concentrations of the chemotherapy to target residual cancer cells while minimizing systemic exposure. The heated solution enhances the absorption and effectiveness of the drug. This combined technique has been shown to improve outcomes in patients by reducing cancer recurrence and extending survival rates. The procedure is complex and requires a highly skilled surgical team, with careful patient selection being essential for the best outcomes.
Cytoreductive surgery combined with HIPEC is best suited for patients with advanced cancers confined to the peritoneum, such as ovarian, colorectal, or appendix cancers. This approach can significantly benefit those whose cancer has not metastasized beyond the abdominal lining. By surgically removing visible tumors and applying heated chemotherapy directly to the affected area, this method aims to reduce tumor burden and target residual microscopic cancer cells. Candidates for this procedure must be carefully assessed based on overall health, cancer type, and stage, as it is an intensive and complex treatment. Successful outcomes often depend on thorough pre-operative evaluation, ensuring that the patient can tolerate the surgery and benefit from the dual treatment approach.
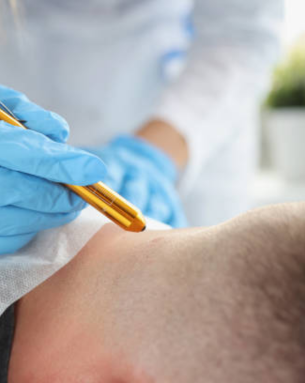
A chemoport is a small, implantable medical device that facilitates the administration of chemotherapy and other intravenous treatments. It is placed under the skin and connected to a major vein, typically in the chest area. This device enables direct access to the bloodstream, reducing the need for repeated needle sticks and minimizing vein damage from frequent infusions. The chemoport helps streamline the treatment process, making it more comfortable and less stressful for patients undergoing long-term cancer care. Its design also allows for safer and more efficient delivery of chemotherapy, ensuring patients receive the full benefit of their prescribed treatments while minimizing discomfort.
Chemoport insertion is a minimally invasive procedure typically performed under local anesthesia, sometimes with sedation. During the procedure, a small incision is made to place the port under the skin, and a catheter is connected from the port to a vein. The entire process usually takes about an hour. Recovery is relatively quick, with most patients resuming normal activities within one or two days. Post-operative care includes keeping the incision site clean and monitoring for signs of infection. Proper port maintenance and flushing are essential to prevent blockage and ensure continued effectiveness. Overall, a chemoport enhances the comfort and convenience of ongoing treatment, improving the patient’s quality of life.
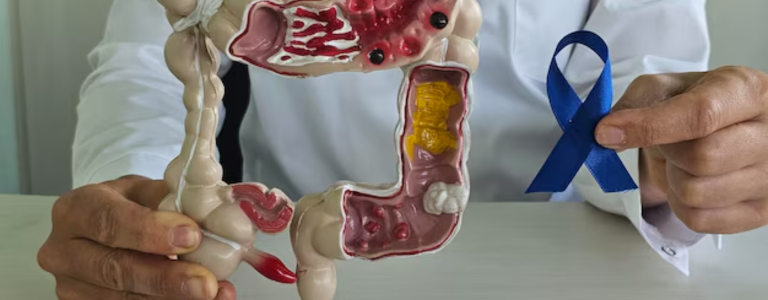
Peritoneal malignancies are cancers that originate in or spread to the peritoneum, the thin membrane lining the abdominal cavity. These can include primary cancers like peritoneal mesothelioma or secondary cancers that have metastasized from the ovaries, colon, or appendix. Treatment often involves cytoreductive surgery to remove visible tumors, followed by HIPEC, where heated chemotherapy is administered directly to the peritoneal cavity. This combined approach targets microscopic cancer cells left behind after surgery, aiming to improve survival rates. Treatment plans are tailored based on the type of malignancy, its spread, and the patient’s overall health to maximize effectiveness and recovery.
Peritoneal malignancies can present with symptoms such as persistent abdominal pain, bloating, unexplained weight loss, and changes in bowel habits. Additional signs may include a feeling of fullness, nausea, and general fatigue. Diagnosis usually requires imaging tests, such as CT or MRI scans, and a biopsy to confirm the presence of cancerous cells. Early detection can significantly influence treatment options and effectiveness, so it is important to seek medical attention for persistent or unusual symptoms. Timely evaluation and intervention can lead to better management and outcomes for patients dealing with peritoneal cancer.
Reconstructive cancer surgery focuses on restoring appearance and function after the removal of tumors. It is commonly performed for cancers affecting areas like the head, neck, breast, and limbs, where aesthetic and functional concerns are significant. This type of surgery may involve skin grafts, tissue flaps, or the use of prosthetics to rebuild structures and support the patient’s physical and emotional recovery. Reconstructive procedures aim to help patients regain confidence, improve daily functioning, and enhance their quality of life. This surgical approach is tailored to the individual’s needs and is often a key part of comprehensive cancer treatment plans.
Reconstructive surgery provides multiple benefits for patients after cancer treatment, both physically and emotionally. It helps restore normal function, enabling patients to speak, eat, or move as naturally as possible, depending on the area treated. Additionally, it plays a crucial role in rebuilding appearance, which can improve self-esteem and overall mental health. Techniques like flap reconstruction, skin grafts, and implant use are tailored to individual needs. Beyond aesthetics, reconstruction can also address structural deficits that could otherwise impact long-term health. By enhancing functionality and appearance, reconstructive surgery supports a holistic recovery, allowing patients to resume their daily activities with greater confidence and comfort.
.png)
.png)

.png)
.png)

.png)





.png)







